Specialist service which uses artificial lung to treat critically ill patients marks one year at UHBW and NBT
Last updated: 11/01/2024
 Left to right: BRI ICU consultant at UHBW, George Townsend, ECMO patient Bethany King, and ECMO Nurse Specialist at UHBW, Carly Smith
Left to right: BRI ICU consultant at UHBW, George Townsend, ECMO patient Bethany King, and ECMO Nurse Specialist at UHBW, Carly Smith
Critically ill patients whose lungs have stopped working properly are being treated using an artificial lung outside the body in Bristol, through a collaborative service between University Hospitals Bristol and Weston NHS Foundation Trust (UHBW) and North Bristol NHS Trust (NBT).
The specialist service, known as veno-venous ECMO (Extracorporeal Membrane Oxygenation), involves a highly complex procedure to support patients who have a critical respiratory condition that prevents the lungs from functioning normally.
An artificial lung located outside the body puts oxygen into the blood and returns it to the body, temporarily doing the work of the lungs and giving them time to heal. Patients treated by ECMO need the temporary life support system as all other types of breathing support have not worked.
The ECMO service recently marked its first year in Bristol, located at the Bristol Royal Infirmary (BRI) Intensive Care Unit (ICU). It is one of only six ECMO centres in England and has treated 16 patients so far, all of which have responded successfully to the treatment. The staff delivering the ECMO service work at either the BRI ICU or Southmead Hospital ICU.
Sanjoy Shah is the Senior Responsible Officer for the Acute Provider Collaborative - Clinical delivery, a programme focusing on working together to plan, deliver, and transform hospital services across the Bristol, North Somerset and South Gloucestershire (BNSSG) area. He said: “ECMO is a highly specialist service we are proud to be offering to seriously ill patients across the South West of England here in Bristol. It is a priority for UHBW and NBT to work together to deliver high quality care in Bristol for patients across the region.
“The ECMO procedure involves inserting two cannulas (tubes) into two veins and placing them near the heart. Blood is then pumped from one tube through an artificial lung, where oxygen is added and carbon dioxide is removed. This allows the oxygen-rich blood to pass back into the patient’s blood stream through the second tube.
“The Bristol ECMO service marking a year of operation is a significant achievement in collaborative working across UHBW and NBT and I want to thank everyone involved in supporting the service over the past 12 months, including Guy’s and St Thomas’ NHS Foundation Trust, Royal Brompton Hospital, Retrieve Adult Critical Care Transfer service and Southmead Hospital Charity.”
The service, which launched in November 2022, was part-funded through a transformational £1.25 million anonymous donation to Southmead Hospital Charity during the Covid-19 pandemic and initially supported patients in the BNSSG area. It expanded its remit to become a regional service in October (2023) to provide a 24/7 retrieval service for the South West of England, working alongside the Royal Brompton Hospital and Guy’s and St Thomas’ NHS Foundation Trust.
Bethany King was one of the first ECMO patients in Bristol. She was first admitted to Southmead Hospital during December (2022) with what was thought to be a chest infection. After being reviewed by a specialist from the Royal Brompton Hospital, it was recommended Bethany was transferred to the specialist care at the BRI for the ECMO treatment.
Bethany said: “Prior and during most of my experience of having ECMO I was extremely unwell and in an induced coma where doctors said it would be touch and go if I survived. As a healthy 20-year-old, this was information my family never expected to hear. Once the ECMO treatment commenced, I started to make small improvements and was slowly woken up from the coma. At the time, I was so desperate to have the ECMO treatment removed as it was limiting me to my hospital bed, and all I wanted to do was get up and go home. However, upon reflection, ECMO along with the brilliant staff at the ICU saved my life and without it I likely wouldn’t be here.
“I will forever be grateful to everyone - there are far too many to name individually - who helped me throughout the whole of my journey and I am so thankful that ECMO was available to me when it was so desperately needed.”
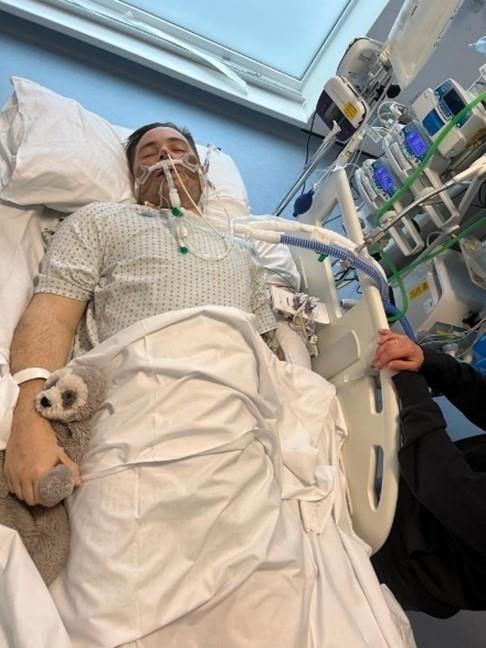
ECMO patient Luke McQuillan undergoing treatment in the BRI ICU
Luke McQuillan was being treated for Type 2 respiratory failure at Swindon Great Western Hospital before he was put into an induced coma and transported to the BRI to undergo ECMO treatment.
Luke said: “I can really only speak for the aftercare as for most of it I was asleep, but having gathered a lot of information from my wife and mum, the care was exceptional. The staff’s focus of course was making sure I was well looked after, but the emotional support they provided for my family was something we’ve never experienced before.
“It is, of course, not a situation anyone wants to find a loved one in, but they certainly made the entire event as easy as one such event can be. My family and I built amazing relationships with many of the BRI team, from the ICU nurses, ECMO nurses, ECMO specialists, doctors and physios - all of them truly going above and beyond.
“Thank you for giving me my life back, for giving my children their dad to celebrate Father’s Days, birthdays and Christmas; giving my wife her husband back and giving my parents their son back. It’s very easy to take life for granted but something like this really makes you realise how fickle life is and how you need to treat every moment as a special one because we were so very close to not being able to share those memories and special moments and dull days together.”
 Councillor Paul Goggin, Lord Mayor of Bristol, with ICU nursing staff at the BRI
Councillor Paul Goggin, Lord Mayor of Bristol, with ICU nursing staff at the BRI
Councillor Paul Goggin, Lord Mayor of Bristol, who was diagnosed with pneumonia in June (2023) which developed into explosive pleurisy (inflammation around the lungs) and later, sepsis, spent three months in the BRI ICU.
He said: “After being rushed to the ED by ambulance and being diagnosed I was cared for in the BRI and underwent an operation, staying in the ward for a couple of weeks. However, when I briefly went back home my symptoms started to get worse and I was rushed back into the Same Day Emergency Care unit. Whilst back on the ward my temperature hit a dangerous 105.9 and while on the ward, the last thing I remember is being in the hospital room, the emergency cord being pulled, sirens going off and lots of staff coming in to help me.
“The next thing I remember was two months later when I woke up in ICU with a tracheostomy. I couldn’t speak or move my arms or legs – it was terrifying. What had happened in the meantime was explained to me later.
“I was told that I must have been fighting it back so hard, that when sepsis struck in the form of a septic shower, it took over my body so quickly. The doctors and nurses were battling to save my life. My partner Debs came back into the room some hours later and I was completely surrounded by the medical team. There was no further progress, and the prognosis was still very grim.
“After returning home, Debs got a call at one in the morning from a consultant and was told I could undergo a procedure and be put onto an ECMO machine. She was talked through what this meant, and the potential risks, but there was no alternative – it was the only way I would survive.
“Thankfully she got another call at four in the morning to tell her that I had survived the initial procedure. Two tubes were inserted into my thighs and I was treated on ECMO for two weeks. During this time, I kept getting further infections and at one point also had to be put on dialysis. Thankfully, I survived the treatment and was able to recover, after subsequently being put into a medical coma for a further two weeks.
“On the ICU, all the staff were amazing. After waking up and having had my muscles waste away to the point where I couldn’t even sit up in bed, it was obvious there was now a massive amount of work to be done to recover. I felt so loved by everyone who was helping me and I felt like everyone was going through the journey with me.
“It was a very strange experience coming into the hospital in sunny June and leaving in cold October, having missed five months of my Lord Mayor role – but I am trying to make up for it now! I’ve since seen the ECMO machine – it's the most unassuming piece of equipment that doesn’t really look like a life-saving machine, but it did indeed save my life. Some people call it the ‘miracle machine’ and for me, it really was. A huge thank you to everyone at the BRI for their love and care, I will remember it for the rest of my life.”
Find out more about the Bristol ECMO service on the UHBW website and NBT website.